An estimated 1 in 3 people grind or clench their teeth — and most of them have no idea.
There’s no pain in the moment. No sensation to wake you. Just a slow, invisible process of enamel erosion happening while you sleep, night after night, until a dentist points to flattened cusps and asks if anyone has mentioned your teeth grinding.
Bruxism is the clinical name for this habit. It’s more common than most people realise, more damaging than it sounds, and more manageable than it might seem — once you understand what’s actually happening and how to protect your teeth from the consequences.
This is everything you need to know.
What Is Bruxism?
Bruxism is involuntary grinding, gnashing, or clenching of the teeth outside of normal chewing function. It can occur during sleep, during waking hours, or both.
The word comes from the Greek brychein — to gnash the teeth. It’s classified as a movement disorder and is recognised by dental and medical communities as a condition worth actively managing, primarily because of the dental damage it causes over time.
Bruxism is not a disease. It’s a behaviour — one that most people engage in unconsciously and cannot stop through willpower alone. That distinction matters because it shapes how we think about managing it. You can’t simply decide to stop grinding. But you can protect your teeth from the damage grinding causes.
Sleep Bruxism vs Awake Bruxism: Two Different Problems
Bruxism comes in two clinically distinct forms, and understanding which one you have — or whether you have both — shapes the management approach significantly.
Sleep bruxism
Sleep bruxism occurs during sleep and is classified as a sleep-related movement disorder. The person has no conscious awareness of it happening. Episodes often occur in clusters across the night, frequently during lighter sleep stages.
Sleep bruxism tends to involve higher force than awake bruxism — the conscious feedback loop that would normally limit how hard you bite is absent during sleep. This is why sleep bruxism causes the most dental damage, and why a protective oral appliance worn at night is the cornerstone of managing its impact on your teeth.
Awake bruxism
Awake bruxism — sometimes called daytime clenching — is more commonly characterised by jaw clenching than grinding. People who do it are often partially aware of the habit, noticing they’re clenching during stressful tasks, long drives, concentrated work, or difficult conversations.
Because the person is conscious, awake bruxism is somewhat more amenable to behavioural interventions — awareness exercises, jaw relaxation habits, stress management. However, it still causes wear and still benefits from protective measures during sleep.
Many people have both forms simultaneously.
| Sleep bruxism | Awake bruxism | |
|---|---|---|
| When it occurs | During sleep | During waking hours |
| Primary behaviour | Grinding + clenching | Predominantly clenching |
| Conscious control | None — happens unconsciously | Partial — can be interrupted with awareness |
| Main triggers | Sleep disruption, stress, medications | Stress, concentration, emotion, habit |
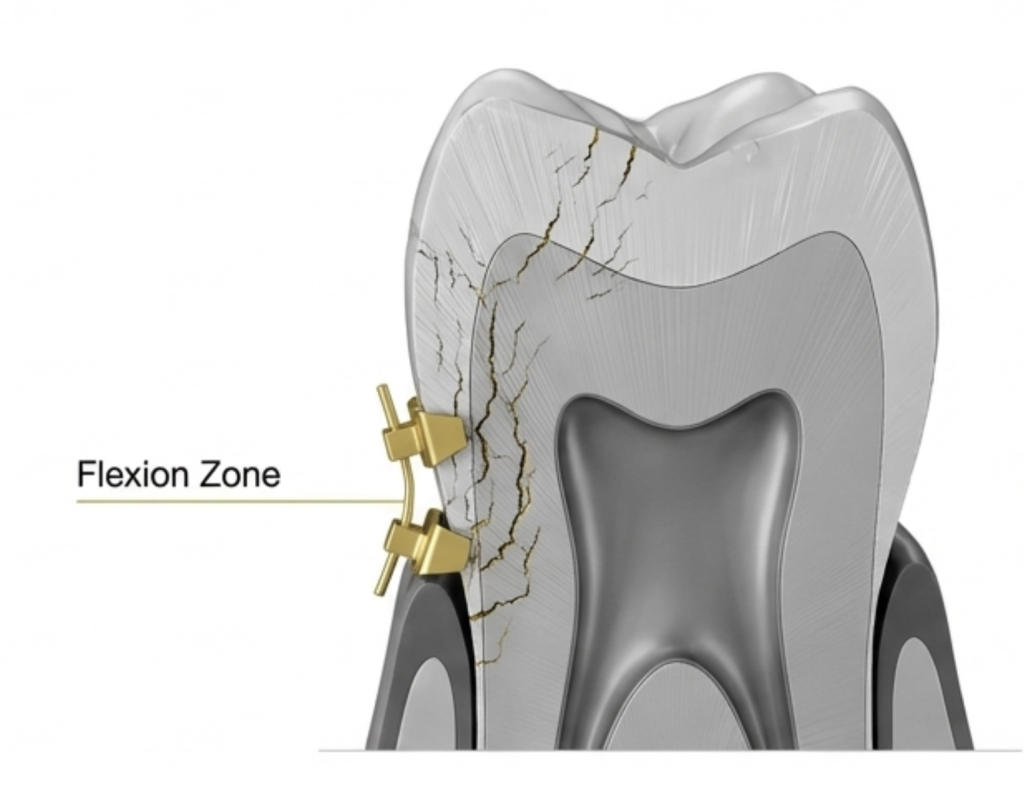
| Wear pattern | Flattened surfaces, worn cusps | Stress fractures, abfraction lesions |
| Audible? | Often — grinding sound | Usually silent |
| Night guard helps? | Yes — primary protection tool | Partially — doesn’t address daytime habit |
Sleep bruxism and awake bruxism are related but distinct — and often occur together in the same person.
What Causes Bruxism?
Bruxism doesn’t have a single cause. Research points to a combination of neurological, psychological, and lifestyle factors — which is partly why it’s difficult to eliminate entirely.
Stress and anxiety
Psychological stress is the most consistently identified contributing factor. The jaw-clenching response appears to be part of the body’s stress activation pattern — the same physiological arousal that prepares the body for threat also increases jaw muscle tension. People under sustained stress or anxiety tend to exhibit more bruxism episodes, both during sleep and while awake.
Sleep disorders
Sleep bruxism is more prevalent in people with other sleep disturbances. There is a well-established association between bruxism and sleep apnea — people with obstructive sleep apnea show significantly higher rates of bruxism. Disrupted sleep architecture appears to create more conditions in which grinding episodes can occur.
Medications and substances
Certain medications are known to increase bruxism, particularly:
- Stimulants — Adderall, Vyvanse, and other ADHD medications commonly increase jaw clenching and grinding as a side effect
- SSRIs and SNRIs — some antidepressants are associated with elevated bruxism rates
- Caffeine — high caffeine intake has been linked to increased grinding activity
- Alcohol — disrupts sleep stages in ways that can increase grinding episodes
If your bruxism began or worsened after starting a new medication, it’s worth discussing with your prescribing clinician.
Genetic factors
Bruxism appears to have a hereditary component. If a parent or sibling grinds their teeth, your likelihood of doing the same is meaningfully higher. Family aggregation studies suggest genetics plays a role in predisposition, though specific genes haven’t been isolated.
Personality and arousal tendencies
People with high baseline arousal levels — competitive, high-strung, perfectionistic personality types — show higher rates of bruxism. This aligns with the stress mechanism: those who are physiologically more activated tend to exhibit more jaw tension.
Symptoms of Bruxism: How to Know If You Have It
Because sleep bruxism happens unconsciously, most people are diagnosed either by a partner who hears them grinding, or by a dentist who spots the evidence. That said, there are symptoms to watch for.
Dental signs
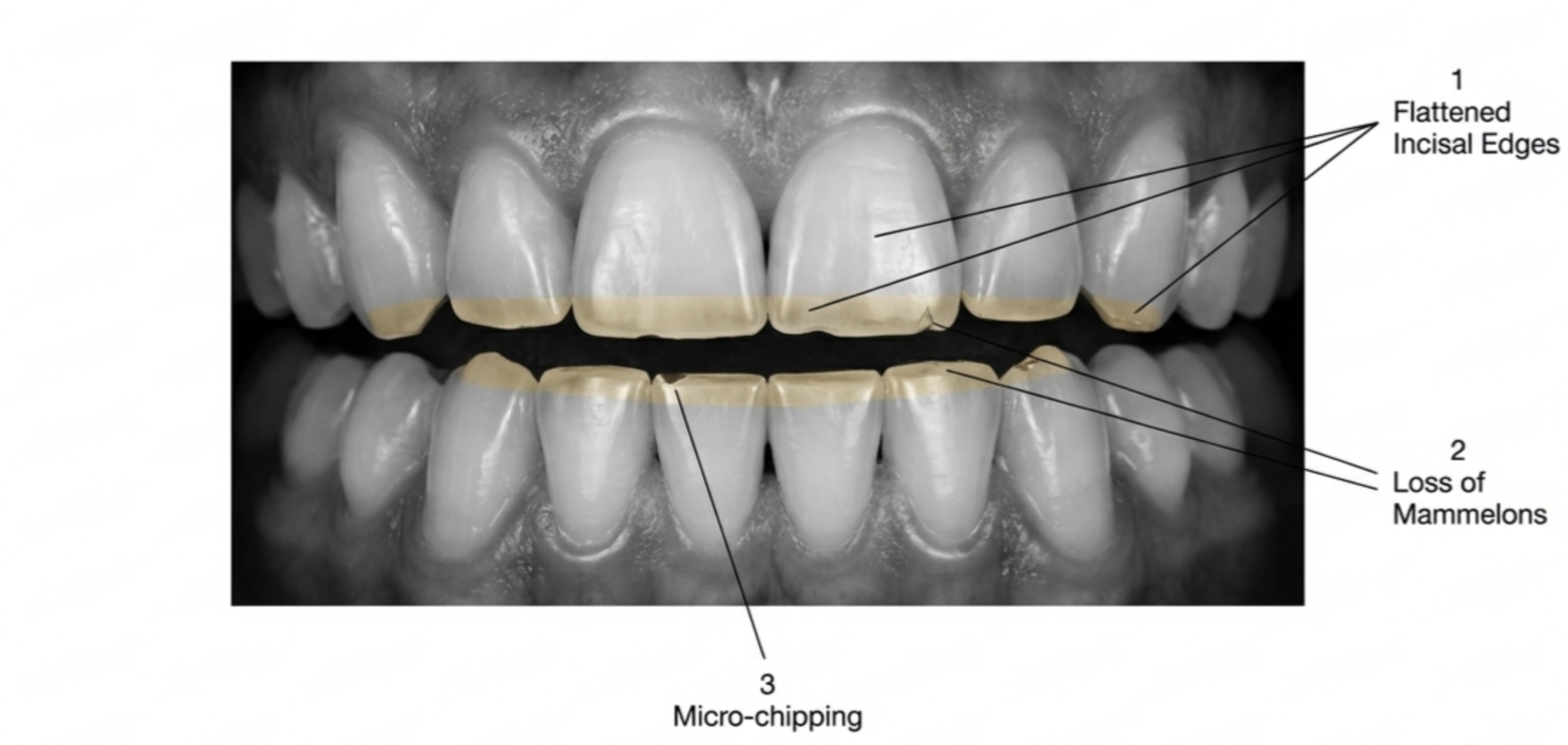
- Flattened, worn, or shortened teeth — the most direct evidence; your dentist can spot this during a routine exam
- Chipped or cracked enamel — particularly on the inner edges of teeth
- Increased tooth sensitivity — as enamel thins, the underlying dentine becomes more exposed
- Indentations on the tongue — from pressing the tongue against teeth during clenching episodes
- Worn-down tooth cusps — the natural peaks of molars become flattened
Physical symptoms
- Jaw muscle soreness or fatigue — particularly in the morning
- Morning headaches — often concentrated at the temples, from sustained jaw muscle tension overnight
- Ear discomfort — tension in the jaw muscles can radiate into the surrounding area
- Facial muscle tightness — the masseter muscles may feel tight or enlarged in heavy grinders
- Disrupted sleep — your own grinding may partially rouse you, even if you don’t fully wake
Partner observation
A sleeping partner hearing grinding sounds is often the first alert. Sleep bruxism episodes can be audible, though many grinding episodes are silent clenches rather than the grating sound most people associate with the habit.
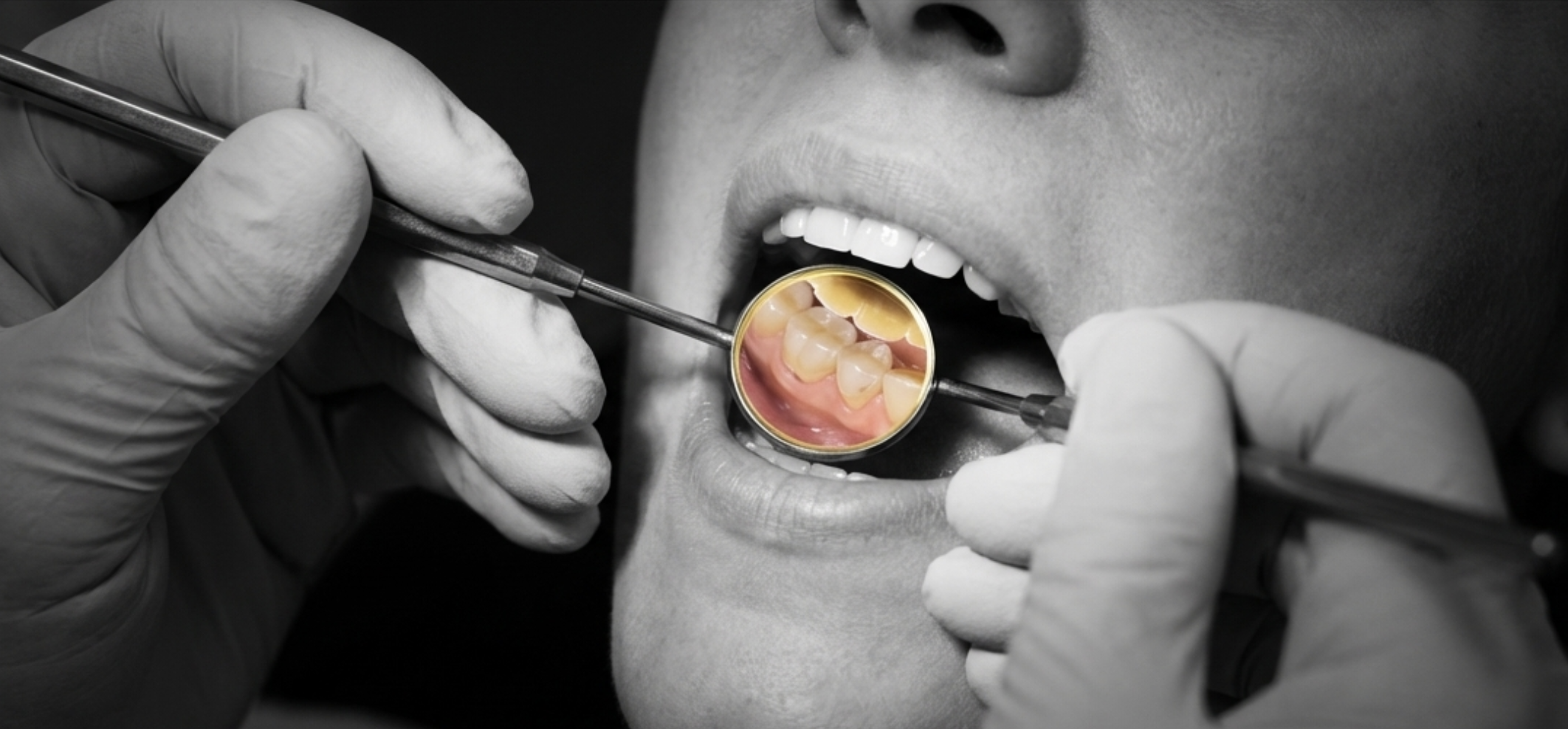
How Bruxism Is Diagnosed
There’s no single definitive test for bruxism. Diagnosis is typically based on:
- Dental examination — your dentist looks for characteristic wear patterns, enamel loss, and muscle changes
- Clinical history — symptoms, sleep patterns, partner observation, medication use
- Sleep study (polysomnography) — for complex cases or where sleep apnea is suspected, a sleep study can confirm and characterise bruxism episodes
For most people, a dental examination combined with symptom history is sufficient for a working diagnosis and the recommendation of protective measures.
Managing Bruxism: What Actually Works
Bruxism has no single cure — but it can be managed effectively. Management typically involves a combination of approaches, with tooth protection as the non-negotiable foundation.
Tooth protection: the oral appliance
An oral appliance — a night guard or bruxism mouth guard worn during sleep — is the primary evidence-based approach to protecting teeth from bruxism damage. It doesn’t stop the grinding, but it absorbs and distributes the force before it reaches your enamel. For anyone with confirmed bruxism, a well-fitted protective appliance is the most important step.
Key factors in appliance effectiveness:
- Material hardness — hard acrylic guards outperform soft guards for moderate to heavy bruxers
- Custom fit — an impression-based fit distributes force correctly across your bite
- Consistent use — protection only works on the nights you wear it
Stress management
Given the strong link between stress and bruxism, approaches that reduce physiological arousal can reduce grinding intensity and frequency — including regular physical exercise, mindfulness and relaxation practices, cognitive behavioural therapy (CBT), and sleep hygiene improvements. These are complementary to tooth protection, not replacements for it.
Addressing contributing factors
If medication is contributing to bruxism, speak with your prescribing clinician. In some cases, a dosage adjustment, timing change, or medication switch can reduce bruxism severity without compromising treatment efficacy. Reducing afternoon caffeine and moderating alcohol can also help reduce grinding episodes.
Biofeedback
Biofeedback devices monitor jaw muscle activity and alert the user when clenching occurs, allowing them to consciously relax the jaw. This shows promise particularly for awake bruxism, where the person can respond to the alert in real time.
Botulinum toxin injections
Botulinum toxin (Botox) injected into the masseter muscle reduces its contractile force, which can reduce grinding intensity in some patients. This is typically reserved for severe cases where other approaches haven’t provided adequate relief, and requires ongoing treatment to maintain effect.
Not sure which appliance is right for your grinding pattern?
Use the Reviv how-to-choose guide →The Dental Damage Bruxism Causes (and Why It Matters)
Understanding what bruxism does to teeth over time is the clearest argument for taking protective measures seriously.
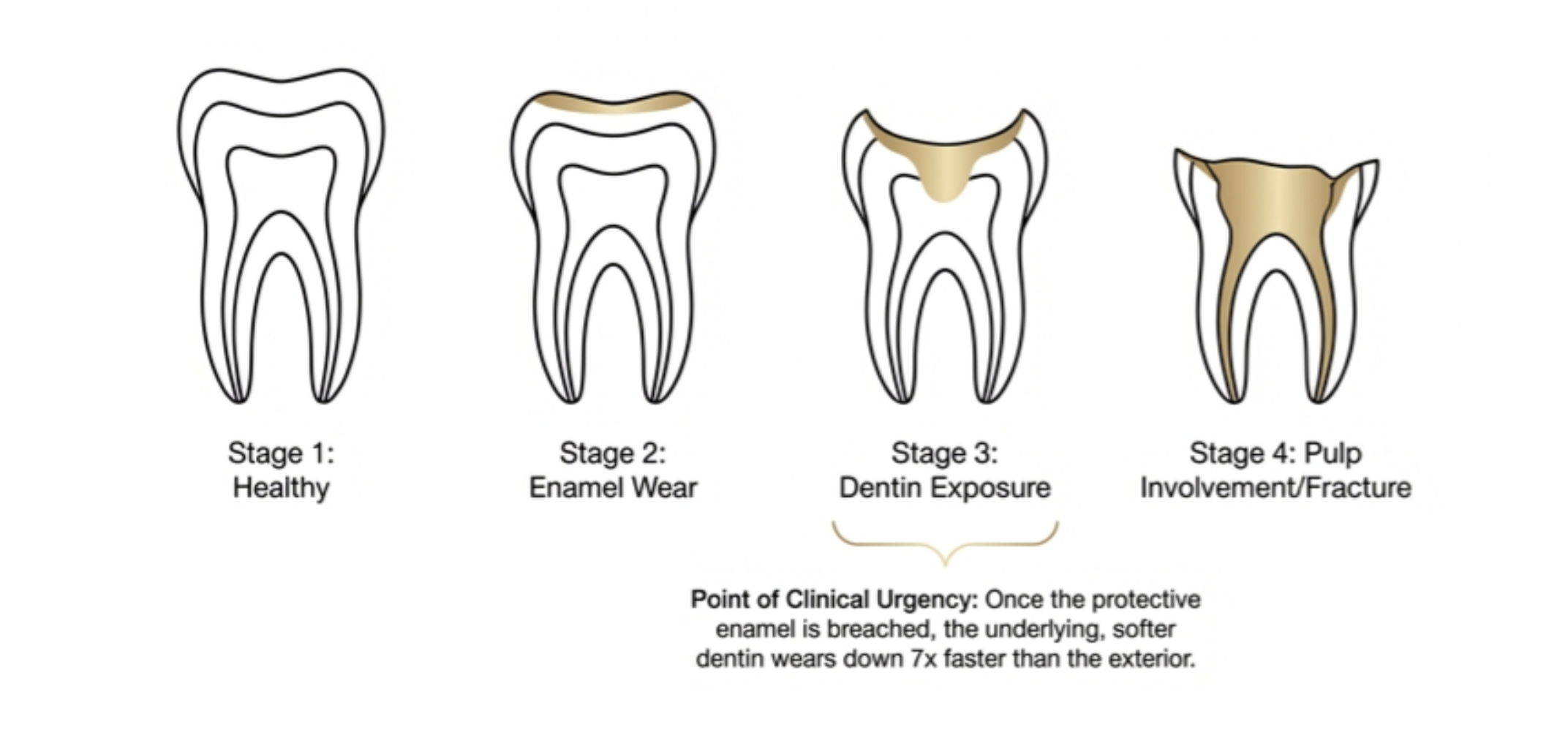
Enamel erosion is the primary consequence. Enamel is the hardest substance the human body produces — but it doesn’t regenerate. Once it’s gone, it’s gone.
Dentine exposure follows enamel thinning. Dentine is softer than enamel and more sensitive. Exposed dentine causes increased tooth sensitivity and is more vulnerable to further wear.
Cracking and fractures — sustained high grinding forces can cause microscopic cracks that deepen over time, eventually leading to visible fractures or full tooth breaks.
Tooth shortening — over years of untreated heavy grinding, teeth visibly shorten. Natural tooth height is lost in ways that affect both function and appearance.
Restoration failure — fillings, crowns, and other dental work are subject to the same grinding forces as natural teeth. Heavy bruxers tend to experience accelerated failure of dental restorations.
The economic argument is straightforward: a protective guard is far less expensive than the restorations and procedures that become necessary after years of unprotected grinding.
When to See a Dentist or Doctor
See your dentist if:
- You’ve been told you grind your teeth by a partner or previous dentist
- You regularly wake up with jaw soreness or headaches
- You’ve noticed increased tooth sensitivity
- You can see visible wear or flattening on your teeth in the mirror
See your doctor if:
- Bruxism started or significantly worsened after beginning a new medication
- You suspect you may also have a sleep disorder (sleep apnea, insomnia, restless legs)
- Jaw or facial discomfort is affecting your daily life
The Bottom Line
Bruxism is a common, involuntary habit that most people have without knowing it. Its causes are multifactorial — stress, sleep disruption, medications, genetics — and there’s no single fix. But its consequences — progressive enamel loss, tooth sensitivity, cracking, and costly restorations — are entirely preventable with consistent protective measures.
A well-fitted oral appliance is the foundation of managing bruxism’s dental impact. Worn every night, it absorbs the force your teeth would otherwise take. Everything else — stress management, lifestyle adjustments, addressing contributing factors — builds on top of that foundation.
If you’ve been diagnosed with bruxism or suspect you grind your teeth, starting with the right protective appliance is the most important step you can take. The Reviv how-to-choose guide helps you find the right fit for your grinding pattern, or browse the full range of FDA-registered Class I appliances designed for grinding protection.
Frequently Asked Questions
What is bruxism?
Bruxism is the involuntary grinding, gnashing, or clenching of teeth outside of normal chewing function. It occurs during sleep (sleep bruxism) or while awake (awake bruxism) and is classified as a movement disorder. Most people who have it are unaware, as it typically happens unconsciously.
What causes bruxism?
Bruxism has multiple contributing causes including psychological stress and anxiety, sleep disorders such as sleep apnea, certain medications (stimulants, SSRIs), high caffeine or alcohol intake, genetic predisposition, and personality traits associated with high physiological arousal. It rarely has a single identifiable cause.
How do I know if I have bruxism?
Common signs include waking up with jaw soreness or headaches at the temples, increased tooth sensitivity, a partner reporting grinding sounds during sleep, and a dentist noticing flattened or worn tooth surfaces at a routine check-up. Many people are first diagnosed by their dentist rather than noticing symptoms themselves.
Can bruxism be cured?
There is no single cure for bruxism. It can be managed through a combination of approaches: a well-fitted oral appliance to protect teeth from grinding force, stress management, addressing contributing medications or lifestyle factors, and in severe cases biofeedback or botulinum toxin injections.
Does a night guard stop bruxism?
No. A night guard does not stop the grinding habit — bruxism is neurological in origin and a physical appliance cannot override it. What a night guard does is protect your teeth from the damage grinding causes by absorbing the force instead of your enamel. Think of it as a helmet: it doesn’t prevent the habit, but it prevents the dental damage.