- What Red Light Therapy Actually Is
- How It Works on Muscle and Joint Tissue
- What the Research Shows for Jaw Pain
- The 2026 RCT in the Journal of Biophotonics
- What It Does Not Do: Bruxism
- Wavelength: What Matters and Why
- Device Types: Clinical vs At-Home
- How to Use It at Home
- How It Pairs With Other Interventions
- The Night Guard Stays
- The Bottom Line
Does red light therapy help jaw pain?
Does red light therapy help with teeth grinding?
What wavelength is best for jaw pain?
How do I use red light for jaw pain at home?
Does red light therapy replace a night guard?
Red light therapy is having its mainstream moment. Devices that cost thousands of dollars in clinical settings are now available for $100–$500 at home. The biohacker community has been using it for muscle recovery and skin health for years. And a growing number of people with jaw pain and bruxism are wondering whether the same technology that reduces muscle soreness after a workout might help with the jaw tension that wakes them up sore every morning.
The honest answer is: probably somewhat, for the right problem — and not at all for what most people with bruxism actually need protection from.
This article covers what red light therapy actually does to tissue, what the clinical research specifically on jaw pain shows, the 2026 RCT that provides the most current evidence, and the clear line between what photobiomodulation can and cannot do for jaw health.

What Red Light Therapy Actually Is
Red light therapy — more precisely called photobiomodulation (PBM) or low-level laser/light therapy (LLLT) — uses specific wavelengths of red and near-infrared light delivered at low power densities that do not cut or heat tissue. The light penetrates into tissue and is absorbed by cellular photoreceptors, triggering biological responses without any thermal damage.
This distinguishes photobiomodulation from surgical and cosmetic lasers, which operate at power levels that deliberately cut or ablate tissue. PBM is non-ablative — the light energy is absorbed and drives cellular processes rather than destroying tissue.
The technology is not new. Low-level laser therapy has been studied in musculoskeletal medicine since the 1970s, and has accumulated a substantial evidence base for pain reduction, muscle recovery, and wound healing across multiple body regions. What is new is the consumer accessibility — the same wavelengths previously available only in clinical devices are now delivered by at-home panels, wands, and targeted devices at price points accessible to general consumers.
How It Works on Muscle and Joint Tissue
The mechanism of photobiomodulation is not fully understood, but the current best-supported model involves primary absorption by mitochondrial chromophores — specifically cytochrome c oxidase, a key enzyme in the mitochondrial electron transport chain. When red and near-infrared light is absorbed, it appears to:
- Increase ATP production — by supporting the electron transport chain, PBM increases the efficiency of cellular energy production in the irradiated cells
- Modulate inflammatory signalling — research shows changes in inflammatory mediators including prostaglandins, interleukins, and reactive oxygen species in irradiated tissue
- Improve local microcirculation — increased nitric oxide release from cells produces vasodilation and improved blood flow to the treated area
- Reduce trigger-point activation — applied to hyperirritable muscle points, PBM has demonstrated reductions in local tenderness and referred pain patterns consistent with trigger-point deactivation
For jaw muscles — particularly the masseter and temporalis, which are among the most metabolically active muscles in the body relative to their size and the most commonly overworked in bruxism — these mechanisms are specifically relevant. A masseter that has been clenching for 8 hours during sleep is metabolically depleted, locally inflamed, and often develops trigger points that produce pain on palpation and referred headache. Photobiomodulation addresses all three of these consequences.

What the Research Shows for Jaw Pain
The evidence base for photobiomodulation in temporomandibular disorders (TMD) is more developed than most people realise. Multiple randomised controlled trials and several systematic reviews have examined its effects on jaw pain, mouth opening, and muscle tenderness.
A 2021 systematic review and meta-analysis in Lasers in Medical Science examined photobiomodulation therapy for TMD pain across multiple trials and found that PBM protocols using red and near-infrared wavelengths significantly reduced jaw pain scores and improved maximum mouth opening compared to sham treatment in multiple patient groups. The effect sizes were moderate — meaningful but not dramatic — and the safety profile was consistently good with no significant adverse effects.
The mechanism that explains why PBM works for jaw pain specifically is the trigger-point and inflammatory pathway: bruxism overloads the masseter and temporalis muscles, producing inflammatory changes and trigger points that generate pain both locally and as referred headaches at the temples. PBM’s anti-inflammatory and trigger-point effects directly address this specific pain pattern.
Important limitations in the existing literature: most studies use clinical laser devices rather than consumer LED panels; many have small sample sizes; and the optimal protocol (wavelength, power density, duration, frequency) has not been definitively established. The research supports efficacy — it does not yet optimise the delivery parameters for at-home use.
The 2026 RCT: What It Found
A March 2026 randomised, controlled, and blinded trial published in the Journal of Biophotonics by Trindade and colleagues provided the most current clinical evidence. The trial used 850nm near-infrared and 660nm red LED clusters — the same combination available in most consumer-grade devices — and found effective pain reduction in patients with temporomandibular disorder compared to a placebo control group.
The significance of this trial is the device type: it used LED clusters rather than laser devices, making it directly translatable to consumer-grade LED panels. Previous research primarily used clinical lasers, which are significantly more powerful and precise than consumer LEDs — making translation to at-home use uncertain. The 2026 trial’s use of LED clusters at consumer-accessible power densities provides the most direct evidence for what the typical at-home user is likely to achieve.
The target sites used in the protocol — the TMJ region and the bilateral masseter and temporal muscles — are the same sites that at-home users would naturally target for jaw pain. The protocol involved six non-consecutive sessions over two weeks, each session applying light to both sites on both sides of the face.
What Red Light Therapy Does Not Do: The Bruxism Distinction
This is the most important section for anyone with bruxism who is considering red light therapy.
Red light therapy does not treat bruxism. There is no randomised controlled trial showing that photobiomodulation reduces the frequency or intensity of teeth grinding. The evidence is for jaw muscle pain and TMJ dysfunction — both of which can be caused or significantly worsened by bruxism — but the grinding behaviour itself is unaffected by photobiomodulation.
The practical implications of this distinction:
- If your jaw is sore in the morning because you ground your teeth all night, red light therapy may reduce that soreness — because it addresses the inflammatory and trigger-point consequences of the overworked muscle
- The grinding that caused the soreness continues unaffected — and while you feel better, your enamel is still being damaged by the unprotected grinding force
- Feeling better does not mean the grinding has stopped or the dental damage has reduced
This is why the framing of red light therapy as a “natural alternative to a night guard” — which appears in some wellness content — is both incorrect and potentially harmful. A night guard protects enamel from grinding force. Red light therapy reduces muscle pain. These are completely different functions addressing completely different consequences of bruxism. The guard is not optional because the soreness has reduced. For the full picture of why distinguishing clenching from grinding matters for protection — the mechanism determines the right guard specification regardless of any adjunct therapy.
Wavelength: What Matters and Why
Not all red light is the same, and the wavelength question is the most important technical variable for someone choosing a device.
Research consistently uses two wavelengths in combination for jaw applications:
660nm — Red light
Visible red light that penetrates to approximately 2–5mm depth, primarily affecting superficial tissue layers including skin, superficial fascia, and the outer portions of muscle tissue. In the jaw context, this wavelength is most relevant for superficial masseter trigger points and the subcutaneous tissue overlying the TMJ. It is the wavelength most commonly associated with general red light therapy panels and is produced by standard red LEDs.
850nm — Near-infrared
Invisible near-infrared light that penetrates to approximately 5–10mm or more, reaching deeper into muscle tissue and joint structures. In the jaw context, this wavelength reaches the deeper masseter muscle belly, the joint capsule of the TMJ, and the retrodiscal tissue behind the joint. For true TMJ joint pain rather than just surface muscle pain, near-infrared is essential — 660nm alone does not reach the joint tissue.
Consumer devices vary enormously in their wavelength specifications. Devices that only produce red light (630–670nm range) will not reach the TMJ joint. Devices that specify both 660nm and 850nm — or near-infrared alongside red — provide the combination consistent with research protocols. This is the specification to look for when evaluating devices for jaw pain specifically.

Device Types: Clinical vs At-Home
Understanding the difference between clinical and consumer devices sets realistic expectations for at-home use.
Clinical laser devices
Most of the existing research uses clinical laser devices — typically Class 3B or Class 4 lasers delivering coherent light at precisely controlled wavelengths. These are significantly more powerful than consumer LEDs, deliver energy more precisely, and are operated by trained clinicians who can target specific anatomical sites with millimetre precision. Clinical laser sessions for TMD are offered at some physical therapy and dental practices.
Consumer LED panels and wands
Most consumer devices use LEDs rather than lasers. LEDs are non-coherent light sources — the light is not as focused or precisely wavelength-controlled as laser light. However, the 2026 Journal of Biophotonics trial specifically used LED clusters rather than lasers and still demonstrated significant pain reduction — providing the most direct evidence that consumer-grade LED devices can produce meaningful effects at jaw-specific target sites.
Consumer devices range from large full-body panels to small handheld wands. For jaw pain specifically, a targeted wand or small panel is more practical than a full-body panel — the application needs to be close to the masseter and TMJ area, which is harder to achieve with a device designed to stand at arm’s length.
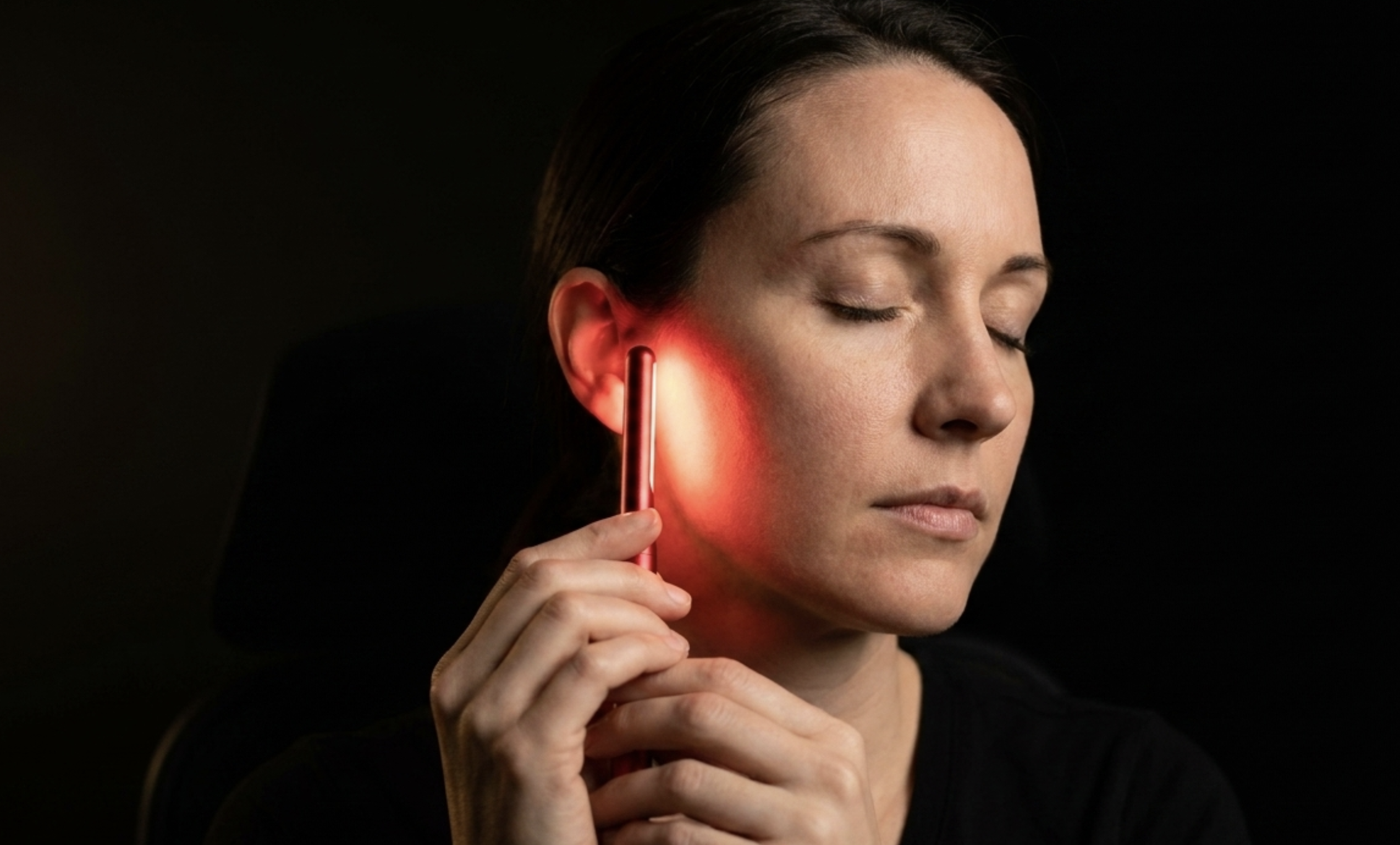
How to Use It at Home for Jaw Pain
The protocol most consistent with clinical research:
Target sites
Two sites per side, four total:
- Masseter — place the device over the large muscle bulk at the angle of the jaw. You can locate this precisely by clenching firmly and feeling where the muscle bulges most prominently
- TMJ — place the device just in front of the ear opening, over the joint itself. You can confirm the location by gently opening the jaw and feeling the condyle move under your fingertip at this site
Duration and frequency
Research protocols typically use 3–6 minutes per site per session. Apply to both sites on both sides — approximately 12–24 minutes per full session. Three sessions per week for two weeks is the most common research protocol. Do not use daily — photobiomodulation requires a recovery window between sessions to avoid the inhibitory effects that occur with overdosing. More is not better; the dose-response relationship is biphasic (too little has no effect; appropriate dose has benefit; too much can inhibit the response).
Pairing with jaw exercises
Research on photobiomodulation for musculoskeletal pain suggests that movement immediately following a PBM session may compound the benefit — the anti-inflammatory and circulation effects make tissue more responsive to therapeutic exercise. Performing the jaw mobility exercises from the TMJ exercise guide immediately following a red light session is a practical application of this principle.
How Red Light Therapy Pairs With Other Interventions
Red light therapy for jaw pain fits into a layered approach that no single intervention can cover alone:
- Red light therapy — addresses inflammation, trigger points, and muscle recovery from bruxism-related overwork. Targets the pain consequence of grinding
- Magnesium glycinate — reduces the neurological clenching drive and muscle excitability that produces the overwork in the first place. The magnesium evidence is the most direct supplement for jaw muscle relaxation
- Jaw exercises — restore mobility and release accumulated trigger points through movement, complementing PBM’s cellular-level effects
- Night guard — protects teeth from grinding force, and may reduce the degree of muscle overwork that requires recovery. The foundational mechanical layer
These four interventions address four different aspects of the bruxism-jaw pain picture without overlap. Using all four produces better outcomes than any one alone — but none of them make the others redundant.
The Night Guard Stays
Red light therapy cannot protect enamel. It can reduce the pain that bruxism causes in jaw muscles. It cannot reduce the wear, cracking, and fracture that bruxism causes in teeth.
Enamel does not regenerate. Once worn away by grinding, it is gone permanently. The cumulative damage of unprotected nightly grinding is irreversible regardless of how well-managed the jaw muscle soreness is. People who use red light therapy to manage their morning jaw pain without wearing a guard are addressing the symptom while the underlying dental damage continues.
If you are grinding your teeth, you need a night guard — a hard custom acrylic guard that absorbs grinding force before it reaches enamel. The soreness management with red light therapy is an appropriate adjunct. It does not change the fundamental calculus of tooth protection.

The Bottom Line
Red light therapy for jaw pain has a legitimate evidence base — stronger than many wellness interventions that receive far more attention. A 2021 systematic review and meta-analysis, and a March 2026 randomised controlled trial in the Journal of Biophotonics, both demonstrate meaningful jaw pain reduction and improved mouth opening with 660nm and 850nm photobiomodulation in TMD patients. The safety profile is consistently good.
The honest assessment: it is a useful adjunct for managing the pain consequences of bruxism — inflammation, trigger points, and morning jaw soreness. It is not a treatment for bruxism itself. It does not stop grinding, does not protect teeth from grinding force, and does not replace a night guard for anyone who grinds their teeth.
The device specification that matters: both 660nm and 850nm wavelengths, applied to the masseter and TMJ, three times per week for two weeks. Consumer LED wands and panels with these wavelength specifications are the category most consistent with the 2026 trial evidence.
For the foundational layer of dental protection: the Reviv model selector identifies the right FDA-registered Class I night guard for your grinding pattern — or browse the full range as the mechanical foundation that any adjunct therapy builds on.