Can a Fitbit detect teeth grinding?
Can an Apple Watch detect bruxism?
Is there a wearable that detects bruxism?
What does low HRV during sleep mean for grinding?
How do I know if I grind my teeth at night?
Google launched the Fitbit Air on May 7, 2026 — a $99 screenless wearable that tracks HRV, sleep stages, SpO2, and sleep scores 24/7. It is Google’s direct answer to WHOOP, and it brings detailed sleep architecture data to a price point accessible to mainstream consumers for the first time.
For the millions of people who grind their teeth at night and don’t know it, or who suspect they might, the question is immediate: can a Fitbit detect teeth grinding? Can any wearable?
The honest answer is no — with an important qualification. No consumer wearable can directly detect teeth grinding. But several of them can detect the downstream signals that bruxism produces in sleep data. Understanding what those signals are, what they mean, and how to act on them is the useful question the Fitbit Air launch actually raises.

The Fitbit Air: What It Actually Measures
The Fitbit Air’s sensor array is directly relevant to this question, so it is worth being specific about what it measures and how:
- Optical heart rate sensor (PPG) — measures heart rate continuously by detecting blood volume changes in the wrist. The Fitbit Air claims 15% better accuracy than previous Fitbit devices for sleep tracking
- Heart rate variability (HRV) — derived from the heart rate data; measures the variation between consecutive heartbeats. HRV is the primary metric used to assess nervous system state — high HRV indicates parasympathetic (recovery) state; low HRV indicates sympathetic (stress/arousal) state
- 3-axis accelerometer + gyroscope — detects movement and body position during sleep
- SpO2 sensor (red and infrared) — measures blood oxygen saturation, useful for detecting oxygen desaturation events consistent with sleep apnea
- Sleep stage analysis — derived from the combination of heart rate, HRV, and movement data; classifies sleep into light, deep, and REM stages
- Skin temperature sensor — detects temperature variation that can indicate illness or menstrual cycle phase
What the Fitbit Air does not have: an electromyography (EMG) sensor. EMG measures electrical activity in muscles — it is the only technology that can directly detect jaw muscle contraction. Without an EMG sensor on or near the jaw, no wrist-worn device can directly measure the masseter activation that constitutes teeth grinding.
What Wearables Actually Measure — And What They Miss
Every consumer wearable on the market — Fitbit, Apple Watch, Oura, WHOOP, Garmin — uses some combination of optical heart rate sensing, accelerometry, and derived metrics. These sensors sit on the wrist or finger and measure cardiovascular and movement signals. They are excellent at inferring sleep architecture from these signals. They are blind to what is happening in jaw muscles on the other side of the body.
The fundamental limitation: bruxism is a jaw muscle event. Its primary signal is masseter and temporalis muscle contraction — electrical activity in specific muscles that can only be detected by sensors placed on or adjacent to those muscles. No wrist or finger device captures this signal.
What wearables can see are the secondary and tertiary consequences of bruxism episodes — the downstream effects that bruxism produces in the cardiovascular and arousal signals these devices do measure:
- Micro-arousal events — bruxism episodes are associated with brief shifts toward lighter sleep, detectable as changes in the heart rate and HRV pattern
- Sleep fragmentation — heavy bruxism produces repeated micro-arousals that reduce time in deep sleep, detectable as a lower deep-sleep proportion in the sleep stage breakdown
- Elevated nocturnal heart rate — the sympathetic activation associated with bruxism micro-arousals produces brief heart rate elevations that show in the overnight heart rate trace
- Reduced HRV — the cumulative arousal burden of a bruxism-heavy night produces lower mean overnight HRV than a bruxism-free night
- Poor sleep scores — the combined effect of the above metrics produces lower sleep scores on any platform that synthesises sleep quality from multiple inputs

HRV and Sleep Fragmentation: The Bruxism Signals
Heart rate variability is the metric most closely associated with bruxism in wearable data, and understanding why helps interpret what you are seeing in your own data.
Bruxism episodes during sleep are preceded by micro-arousals — brief shifts toward lighter sleep that elevate sympathetic nervous system activity. This sympathetic activation reduces HRV in the surrounding sleep window. In a heavy bruxer with multiple episodes per hour, the cumulative effect is significantly suppressed overnight HRV compared to a bruxism-free night.
Research on sleep bruxism has documented this pattern: nights with higher bruxism episode frequency correlate with lower HRV and more fragmented sleep architecture in polysomnography data. The correlation exists because the same physiological event — the micro-arousal — drives both the bruxism episode and the HRV suppression.
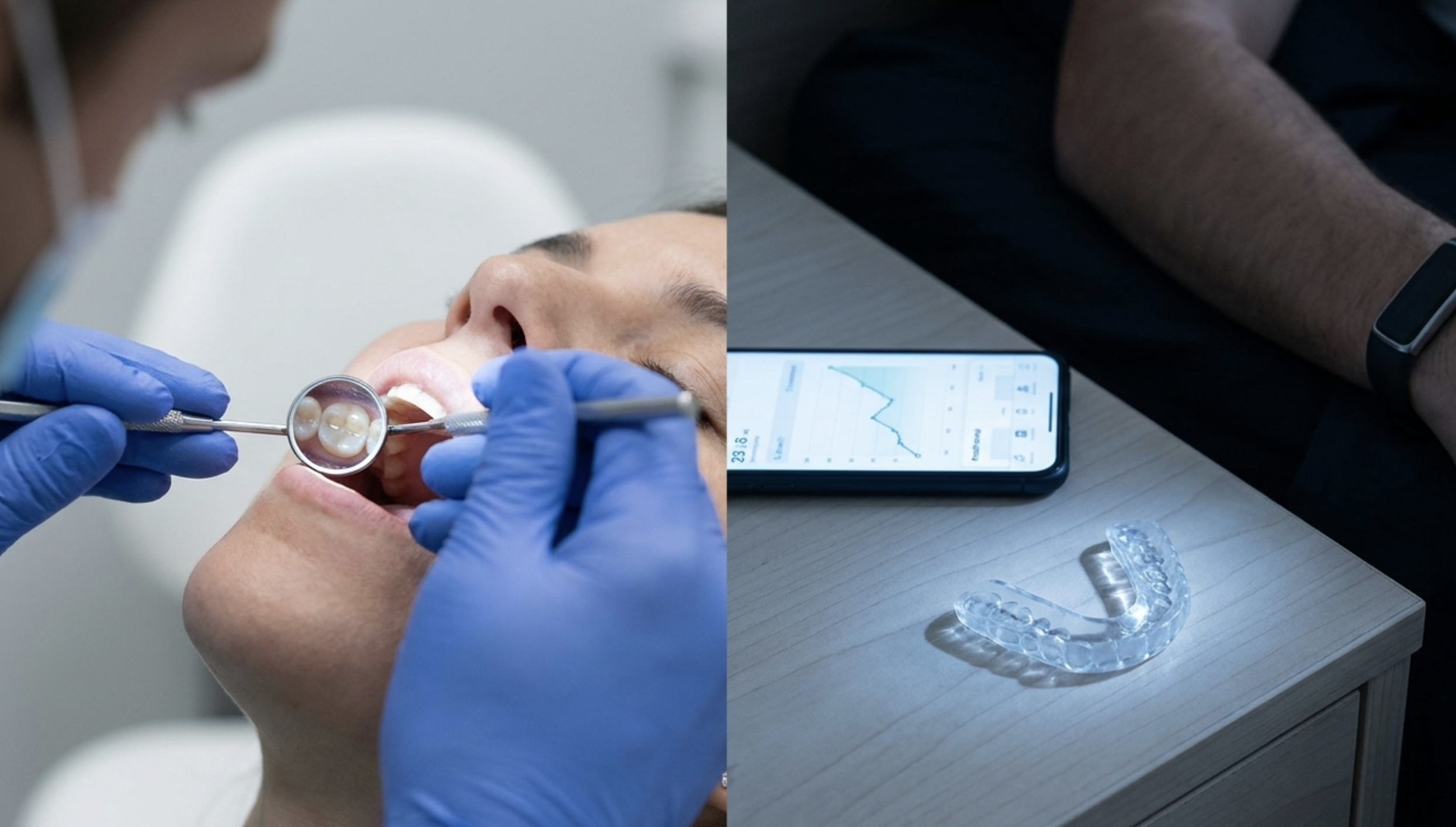
The practical implication for Fitbit Air users: if you consistently see low overnight HRV, high numbers of “arousal” or “restless” events in your sleep data, low deep-sleep proportions, and poor sleep scores despite adequate sleep duration — bruxism is a plausible explanation alongside other possibilities.
The critical caveat: these signals are not specific to bruxism. Obstructive sleep apnea produces identical patterns — and bruxism and sleep apnea co-occur at elevated rates (33–54%). Chronic stress, alcohol, some medications, and poor sleep environment produce similar HRV suppression and sleep fragmentation. A wearable showing these patterns raises the question; it cannot answer it.
Device-by-Device: What Each Wearable Can Tell You
Fitbit Air (Google, 2026)
The newest and most relevant to this article’s timing. Can detect: sleep stage fragmentation, overnight HRV, SpO2 desaturation events (useful for identifying OSA-driven arousal), sleep score. Cannot detect: jaw muscle activity, direct bruxism confirmation. Most useful bruxism signal: the combination of consistently low overnight HRV and reduced deep sleep proportion over multiple nights. The SpO2 sensor also provides a useful screen for oxygen desaturation events that suggest sleep apnea — which co-occurs with bruxism and is worth distinguishing.
Apple Watch (Series 9 / Ultra 2)
Can detect: sleep stages, heart rate, blood oxygen, movement. Cannot detect: jaw muscle activity. Most useful bruxism signal: the Health app’s sleep data showing consistently elevated resting heart rate during sleep and fragmented sleep architecture. The Apple Watch’s ECG function is not useful for bruxism but is relevant to cardiac monitoring.
Oura Ring (Gen 4)
The Oura Ring is among the most accurate consumer sleep trackers for physiological measurement. Its finger position provides a stronger PPG signal than wrist devices, producing more accurate HRV and heart rate data. Can detect: sleep stages, HRV (with high accuracy), temperature deviation, SpO2. Cannot detect: jaw muscle activity. Most useful bruxism signal: the Oura HRV data during deep sleep is particularly relevant — deep sleep HRV suppression is a characteristic pattern of bruxism nights. The Oura Readiness Score may also reflect the cumulative effect of chronic bruxism-related sleep disruption over weeks.
WHOOP 5.0
WHOOP’s primary differentiation is HRV monitoring and recovery scoring. Can detect: HRV, sleep stages, respiratory rate, SpO2. Cannot detect: jaw muscle activity. Most useful bruxism signal: WHOOP’s Strain and Recovery metrics may reflect the cumulative parasympathetic deficit from chronic bruxism-related sleep disruption — low recovery scores that don’t improve despite adequate sleep are a signal worth investigating.

Dedicated Bruxism Detection: What Actually Works
Clinical and research-grade bruxism detection uses EMG — electromyography — sensors placed directly over the masseter or temporal muscles. These sensors measure the electrical activity in the jaw muscles in real time, producing a direct readout of grinding and clenching events with millisecond precision.
The BruxOff is the most well-known research device specifically designed for bruxism recording — a wearable EMG device that records masseter activation during sleep and produces a quantified bruxism event count for clinical assessment. It is used in research protocols and clinical practice for the same purpose a polysomnography (sleep study) serves for sleep apnea: direct, measured confirmation.
Academic research has also used adhesive EMG patches placed over the masseter, connected to recording equipment, for overnight bruxism quantification. These protocols produce the gold-standard data that researchers use to validate other detection methods.
None of these are consumer products at consumer prices. The BruxOff is a clinical tool; EMG patches are research equipment. Consumer wearable technology has not yet produced a mainstream device that directly measures jaw muscle EMG during sleep — although this is a logical next frontier as wearable sensors continue to miniaturise. For now, the consumer wearable space offers downstream inference, not direct detection.
How to Interpret Your Own Sleep Data for Bruxism Signals
If you track sleep with any of the devices above and want to identify whether bruxism might be a contributing factor to poor data, look for this combination:
The pattern that suggests bruxism involvement
- Consistently poor sleep scores despite sleeping 7–9 hours — not occasional poor nights, but a consistent pattern over weeks
- Low deep sleep proportion — regularly under 15% of total sleep time in deep/N3 sleep
- Suppressed overnight HRV — particularly if HRV is notably lower during the second half of the night when bruxism episodes tend to concentrate
- High restlessness or arousal counts — frequent micro-movements or arousal flags in the sleep breakdown
- Morning symptom correlation — the nights with worst wearable data also produce the most jaw soreness, temple headaches, or tooth sensitivity in the morning
The pattern that suggests sleep apnea rather than (or in addition to) bruxism
- SpO2 desaturation events — drops below 90–94% during sleep, detectable on Fitbit Air, Oura, and WHOOP
- Loud snoring reported by a partner alongside the poor data
- Daytime fatigue that doesn’t improve with longer sleep
- Witnessed breathing pauses during sleep
Sleep apnea and bruxism co-occur at 33–54% — both may be present simultaneously, each worsening the other’s sleep disruption signature. If the data suggests both, clinical evaluation for both is appropriate. The airway-bruxism connection is covered in detail, including when sleep apnea screening is indicated alongside bruxism evaluation.
How to Actually Confirm Bruxism
A wearable identifies a pattern. A dental exam confirms or rules out bruxism.
The dental confirmation of bruxism uses physical evidence that no wearable can provide:
- Enamel wear patterns — the characteristic flattening of cusps, wear facets on biting surfaces, and enamel loss at the gumline that years of grinding produces. A dentist can date and grade the severity of wear based on its pattern and extent
- Tooth fractures and craze lines — hairline fractures in enamel and cusp fractures that result from repeated grinding force
- Masseter hypertrophy — a visibly or palpably enlarged masseter muscle from years of heavy clenching, visible from the facial profile
- Jaw muscle tenderness — tenderness on palpation of the masseter and temporalis muscles, a reliable clinical indicator of overworked jaw muscles
- Dental restoration damage — crowns, fillings, and veneers showing wear or fracture patterns inconsistent with normal occlusal use
Tell your dentist that you are tracking your sleep with a wearable and are concerned about bruxism. Show them the data if you can — most dentists are now familiar with wearable sleep data and can use it as contextual information alongside clinical examination. The combination of wearable data showing consistent sleep fragmentation and clinical examination finding wear patterns is more diagnostically informative than either alone. For understanding whether clenching or grinding is the primary pattern — the distinction matters for the right guard specification.
What to Do Once You Suspect It
The wearable data has identified a pattern consistent with bruxism. The morning symptoms are consistent. You have an appointment with your dentist. The parallel question is: what do you do in the meantime?
If the pattern in your wearable data is consistent with bruxism — particularly if you have morning jaw soreness alongside the sleep data — starting with a night guard before clinical confirmation is not unreasonable. A hard custom guard worn on the assumption that bruxism may be occurring provides dental protection during the confirmation period. If bruxism is confirmed, the guard was the right choice. If it turns out not to be bruxism, wearing a well-fitted guard for a few weeks while you get a dental opinion causes no harm.
What to avoid: using the wearable data as a substitute for the dental exam. The wearable signals bruxism. The dental exam confirms and grades it. The guard protects from it. All three have roles that none of the others can fill.
One genuinely useful application of wearable data in bruxism management: tracking the effect of interventions. If you start wearing a night guard, you can observe whether your sleep data improves — lower arousal counts, improved HRV, higher sleep scores — as the bruxism-related micro-arousals reduce. This is not a clinical measurement, but it provides useful real-world feedback that the guard is having an effect on sleep quality beyond just dental protection.

The Bottom Line
The Fitbit Air launch brings detailed sleep architecture data — HRV, sleep stages, SpO2, sleep scores — to a $99 price point that removes the barrier for mainstream consumers. It is an excellent sleep tracker. It cannot detect teeth grinding.
What it can detect — and what every serious wrist and finger wearable can detect — are the downstream signals bruxism leaves in sleep data: fragmented sleep architecture, suppressed HRV, reduced deep sleep, high arousal counts. These signals are not specific to bruxism, but in combination with morning symptoms they constitute a meaningful signal worth investigating.
The investigative path is straightforward: note the wearable pattern over multiple weeks, cross-reference with physical symptoms, tell your dentist, bring the data. The dentist confirms or rules out bruxism through clinical examination. If confirmed, a hard custom night guard is the foundational protective step — and you can use the same wearable to track whether sleep quality improves once protection is in place.
The Reviv model selector identifies the right FDA-registered Class I guard for your specific clenching and grinding pattern — or browse the full range. And if your Fitbit Air is telling you something is disrupting your sleep, your dentist is the right next conversation.